Cardiovascular Disease:
A National Crisis
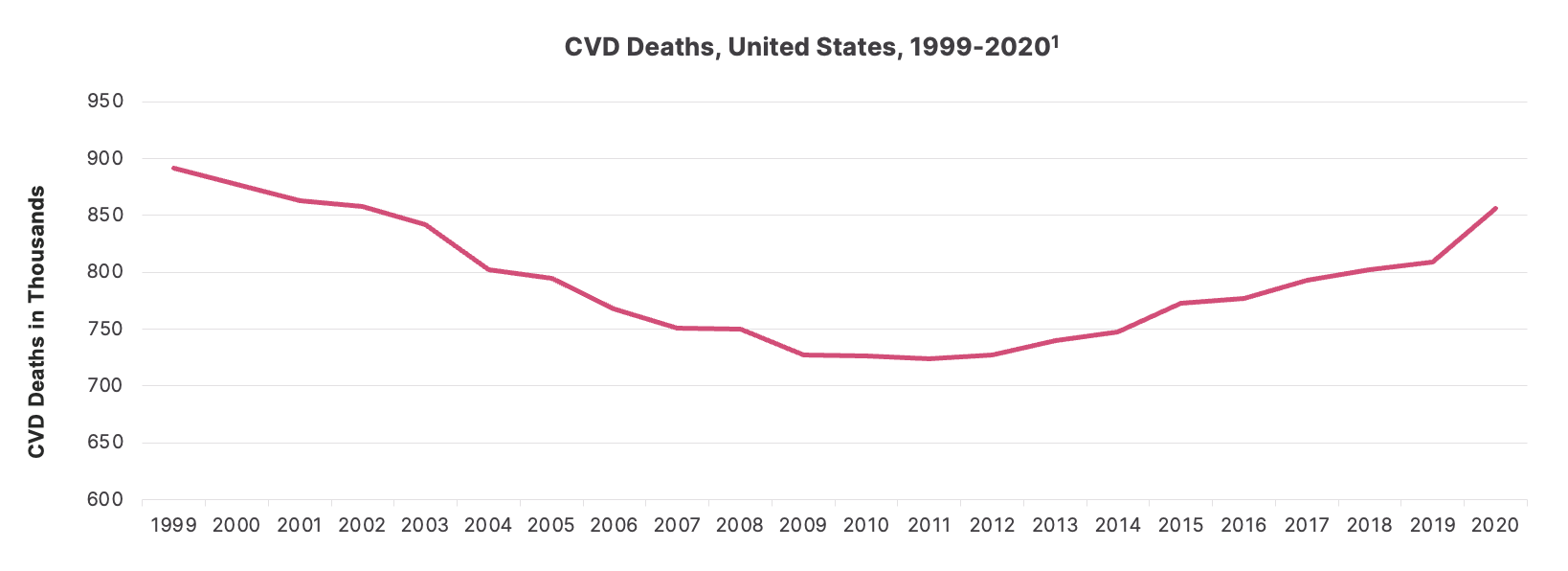
Cardiovascular disease is the number one cause of death for Americans, and it’s on the rise after decades of decline.1
Cardiovascular disease is the number one cause of death for Americans.
Cardiovascular disease (CVD) is the number one cause of death for Americans, killing more people each year than all forms of cancer and accidents combined. It’s also the costliest condition among all major disease categories, accounting for 12% of total U.S. health expenditures and costing the U.S. economy a total of $378 billion each year, including $226 billion in direct health care spending and $152 billion in indirect costs associated with lost productivity.1
Cardiovascular disease is a spectrum of conditions involving the heart and blood vessels that can lead to heart attack and stroke. The most common and deadliest form of cardiovascular disease, atherosclerotic cardiovascular disease or ASCVD, currently affects more than 22 million people – 8% of the U.S. population.2 A multitude of risk factors contribute to the development and progression of ASCVD including high LDL-C (“bad cholesterol”) cholesterol, smoking, high blood pressure, and obesity.
Take Health to Heart: A Policy Agenda to Stop Cardiovascular Deaths
Cardiovascular disease is a national crisis that affects millions of Americans and their families. We must take action now to address the access barriers that lead to poor outcomes like heart attack, stroke, and death.
As organizations working to advance cardiovascular health and the interests of medically underserved communities, the Foundation of the National Lipid Association and the National Medical Association are coming together through Take Health to Heart. Through our initiative, we seek to educate policymakers, providers, patients, and their families about the critical access barriers that lead to poor outcomes and advocate for policy changes at the state and federal levels that can help reverse the alarming trend in cardiovascular deaths.
Our policy agenda is driven by four key priorities we believe are necessary to lead to lasting change in cardiovascular outcomes:



About Us
Take Health to Heart is an advocacy and education initiative of the Foundation of the National Lipid Association and the National Medical Association. Take Health to Heart is made possible through a sponsorship from Novartis Pharmaceuticals Corporation.